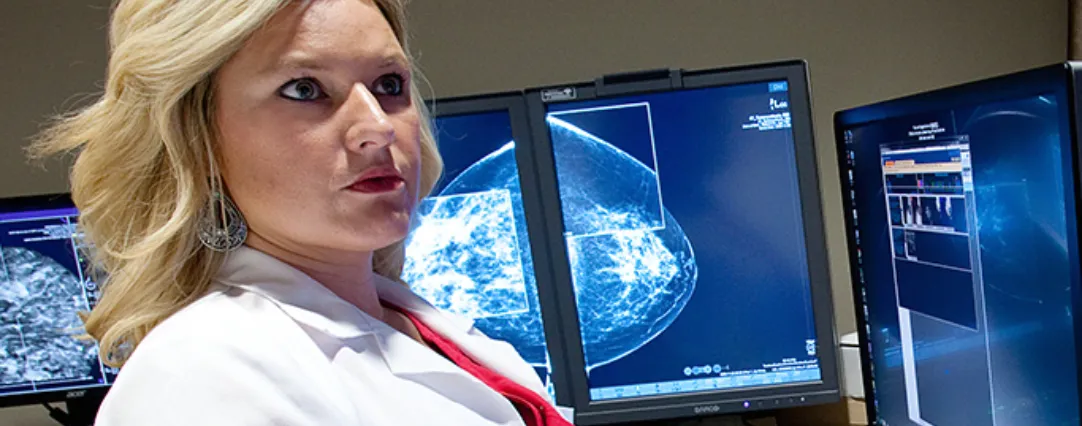
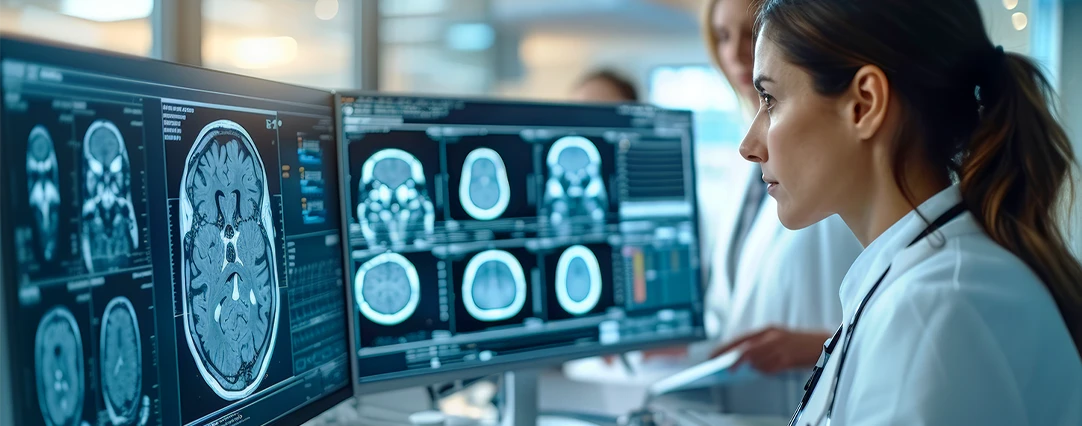
Interventional radiology is changing how some of the most difficult cancers are being treated. At Radiology Associates of North Texas (RADNTX), our subspecialty-trained vascular and interventional radiologists are at the forefront of these exciting developments, making a difference in the lives of area residents every day.
Unlike traditional surgical approaches for treating cancer, the field of interventional oncology uses image-guided, minimally-invasive techniques to directly target cancers, with fewer side effects and better results. Even inoperable cancers are now targeted and treated by specially trained radiologists who guide and administer these treatments using tiny catheters and wires.
RADNTX currently has over 20 fellowship trained interventional radiologists providing services at liver and kidney transplant centers, Level 1 trauma centers, stroke centers and regional  and community medical centers. Our subspecialty experience and area-wide coverage gives Dallas-Fort Worth patients access to the most highly advanced, minimally invasive procedures available.
and community medical centers. Our subspecialty experience and area-wide coverage gives Dallas-Fort Worth patients access to the most highly advanced, minimally invasive procedures available.
The Interventional Oncology treatments performed by our interventional radiologists are broken down into two categories: embolization and ablation.
Tumor embolization is a minimally invasive, palliative procedure that blocks blood supply to tumors. Palliative care means treatments that make the patient feel better and improve quality of life; it is not a cure. Using fluoroscopic guidance, an interventional radiologist performs an angiogram to map out the patient’s anatomy and determine which blood vessels are feeding the tumor. The physician will then advance a catheter to the target vessel to deliver either chemotherapy or radioactive beads designed to kill the tumor and block the bloo
d supply that is feeding the tumor at the same time. These procedures are known as chemoembolization and radioembolization.
Tumor ablation is a minimally invasive, curative (intended to cure), localized treatment that targets and kills diseased tissue with either heat or cold gas while sparing the healthy tissue. The three types of ablation are radiofrequency ablation (RFA), microwave ablation and cryoablation.
In radiofrequency ablation, the interventional-radiologist guides a small needle through the skin into the tumor using image guidance. Radiofrequency energy is transmitted from the needle into the tumor, where it produces heat and kills the tumor cells. With microwave ablation, a microwave antenna is guided through the skin into the tumor using image guidance. From the tip of the antenna, microwave energy is transmitted to the tip of the needle, where it produces heat in the tissues. In both, the dead tumor tissue shrinks and slowly forms a scar. In cryoablation, a probe is guided through the skin into the tumor using image guidance. Instead of killing the tumor with heat as in RFA or microwave ablation, cryoablation uses an extremely cold gas to freeze it. The “ice ball” that is created around the needle grows in size and destroys the frozen tumor cells.
 Although radiofrequency ablation has been used for years to treat various health problems, including back and neck pain as well as varicose veins, the procedure has recently proven very effective at treating the severe pain that can result from spinal tumors.
Although radiofrequency ablation has been used for years to treat various health problems, including back and neck pain as well as varicose veins, the procedure has recently proven very effective at treating the severe pain that can result from spinal tumors.
Using imaging guidance, interventional radiologists target spinal tumors by delivering radiofrequency (RF) energy to the tumor. This heats up and destroys the tumor cells that are causing severe pain in the spine. The procedure creates a cavity that is filled with medical grade cement, helping to stabilize the affected vertebra. RADNTX radiologists use the Spinal Tumor Ablation with Radiofrequency (STAR) system to treat tumors that have spread to the spine.
Radioembolization is one of the most promising advances in the treatment of liver cancer. Liver tumors are among the most difficult to treat, and patients often have a short life expectancy after diagnosis, just a few years in many cases. The minimally invasive treatment, called Selective Internal Radiation Therapy (SIRT) or Y-90 radioembolization, can add years to the lives of patients with inoperable liver tumors while also giving them a better quality of life.
During SIRT treatment, millions of SIR-Spheres® microspheres are delivered through blood vessels directly to the tumor site. The treatment, which can be delivered along with chemotherapy, is done on an outpatient basis, with most patients returning home four to six hours after the procedure.
Y-90 stands for the radioactive isotope Yttrium-90, which is packaged into tiny spheres and delivered through a catheter from the groin into the artery supplying blood to the tumor. SIRT radioembolization uses a higher but more targeted dose of radiation, which spares healthy tissue and results in fewer side effects compared to standard cancer treatments. Most patients experience fatigue for seven to 10 days after the treatment, and some patients may experience mild nausea and abdominal discomfort for 24-48 hours following the procedure.
RADNTX remains committed to providing the most advanced minimally invasive cancer therapies in the Dallas-Fort Worth area, offering embolization and ablation procedures at hospitals across the region.
For more information, visit our interventional oncology page.
Posted: April 17, 2017